
Over the past 15 years, the field of hematopoietic stem cell transplantation has undergone a profound transformation, largely driven by breakthroughs in haploidentical transplantation. Represented by the “Beijing Protocol” pioneered by Professor Xiaojun Huang and his team at Peking University People’s Hospital, haploidentical transplantation has not only overcome the long-standing limitation of donor availability but has also achieved outstanding outcomes in the treatment of hematologic malignancies, leading to its widespread adoption worldwide. This success has further expanded its application from malignant diseases to rare conditions such as severe aplastic anemia and thalassemia. During the 52nd EBMT Annual Meeting, at the “7th EBMT Global Committee Scientific Session: Addressing Unmet Needs Worldwide,” Professor Huang presented a comprehensive report on haploidentical transplantation in rare diseases. He systematically reviewed the latest data and clinical experience from his team and global collaborators, highlighting optimized strategies based on the Beijing Protocol, efficacy outcomes across different diseases, and its unique advantages compared with other transplant approaches. His work provides valuable insights for clinical practice and future development in this field.
Severe Aplastic Anemia
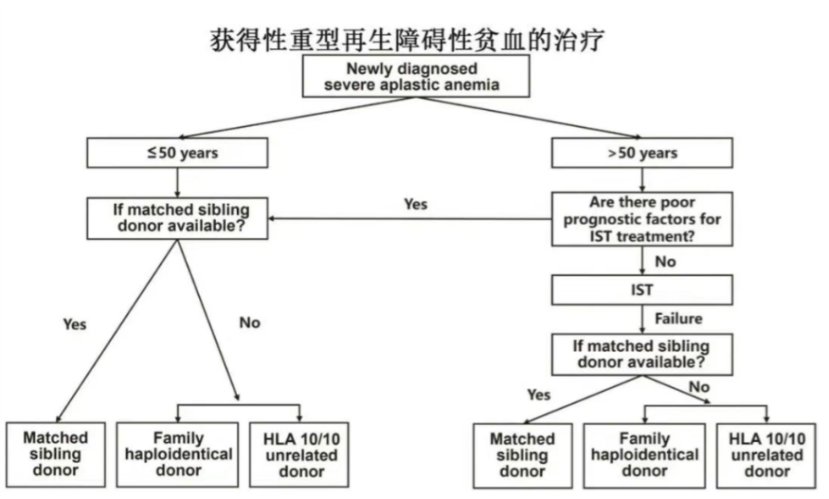
Among the rare diseases explored with haploidentical transplantation, severe aplastic anemia (SAA) has been one of the most significant breakthroughs. Traditionally, treatment options for SAA were limited to immunosuppressive therapy or matched sibling transplantation in younger patients.
Professor Huang’s team innovatively modified the conditioning regimen by adding busulfan to the standard cyclophosphamide and ATG backbone to enhance engraftment. Although initially there were concerns about increased bone marrow toxicity, clinical outcomes demonstrated nearly 100% stable engraftment, laying a strong foundation for treatment success.
Subsequent multicenter studies with large cohorts further confirmed the efficacy of this approach. Patients undergoing haploidentical transplantation achieved overall survival (OS) and failure-free survival (FFS) rates close to 90%, comparable to those receiving matched sibling transplants. Importantly, long-term follow-up of up to nine years showed that quality of life was equivalent between the two groups, indicating sustained high-quality survival.
Based on these robust data, haploidentical transplantation has been incorporated into Chinese guidelines as a first-line treatment option for SAA patients under 50 years of age, alongside matched sibling transplantation. This represents a major shift from previous guidelines that typically restricted matched transplantation to patients under 40. Notably, studies also suggest that donor age may be more critical than HLA matching in this setting, with younger haploidentical donors potentially offering better outcomes than older matched sibling donors.
In contrast, the increasingly popular post-transplant cyclophosphamide (PTCy) approach still has limitations in SAA. Existing data show relatively low engraftment rates of around 67%, which improve to 94% when combined with low-dose ATG, but with a one-year OS of only 81%, significantly lower than the approximately 90% nine-year OS observed with the Beijing Protocol. EBMT data from 2025 also indicate that donor type influences outcomes with PTCy, further reinforcing the advantages of the Beijing Protocol in this setting.
Thalassemia and Other Rare Diseases
Extending the success of haploidentical transplantation to other rare diseases has been another major focus of Professor Huang’s team and the Chinese hematology community. Thalassemia, which has a relatively high prevalence in China, imposes a significant burden on patients and society.
Drawing on extensive experience in leukemia and SAA, Professor Huang’s team developed a tailored conditioning regimen for thalassemia, incorporating busulfan, ATG, fludarabine, hydroxyurea, and cyclophosphamide. Data from more than 800 patients demonstrate nearly 100% engraftment rates across haploidentical, matched sibling, and matched unrelated donors, with a rejection rate as low as 0.5% and a two-year OS of 95%.
Although the incidence of graft-versus-host disease (GVHD) is slightly higher in haploidentical transplantation compared with matched sibling transplantation, the rate of severe acute GVHD remains low and comparable between groups at approximately 10%. These findings indicate that, with well-designed conditioning regimens, haploidentical transplantation can provide safe and effective treatment for thalassemia. In contrast, the application of PTCy in this disease still requires further evidence.
Beyond SAA and thalassemia, haploidentical transplantation has also shown promising results in other rare hematologic disorders. In paroxysmal nocturnal hemoglobinuria (PNH), data from the Chinese Blood and Marrow Transplant Registry (CBMTR) indicate survival rates exceeding 90% in younger patients and around 70% in older patients undergoing haploidentical transplantation. No significant differences were observed between ATG alone and ATG combined with PTCy for GVHD prevention. Recent multicenter studies have further confirmed the effectiveness of the Beijing Protocol in PNH, with manageable rates of severe GVHD despite a slightly higher overall incidence.
In Fanconi anemia, haploidentical transplantation has achieved engraftment rates of up to 96% and a five-year OS of approximately 80%, although GVHD remains a challenge. Additionally, T-cell depletion combined with PTCy has shown potential in PNH treatment. Ongoing research is exploring the broader application of T-cell depletion–based haploidentical transplantation strategies in various genetic diseases to achieve safer and more precise individualized therapies.
Conclusion
Haploidentical hematopoietic stem cell transplantation, particularly the Beijing Protocol, has successfully expanded from the treatment of hematologic malignancies to rare diseases, demonstrating broad clinical potential.
Through disease-specific optimization of conditioning regimens, this approach has achieved long-term survival and quality of life comparable to matched sibling transplantation in severe aplastic anemia, while also delivering encouraging results in thalassemia, PNH, Fanconi anemia, and other challenging rare diseases.
Importantly, this strategy has brought curative treatment opportunities to patients who previously lacked suitable donors. Supported by large-scale, long-term evidence, it is reshaping treatment guidelines and clinical decision-making, offering more flexible and scientifically grounded approaches to age limits and donor selection.
Looking ahead, continued advances in transplant immunology and further refinement of conditioning strategies are expected to enhance outcomes even further. Haploidentical transplantation is no longer limited to malignant diseases—it is becoming a cornerstone in transforming the treatment paradigm of rare diseases and advancing the goal of cure. Its significance lies not only in technological innovation but also in embodying a fundamental medical principle: that every patient deserves access to effective treatment.



Expert Profile

Professor Xiaojun Huang National Clinical Research Center for Hematologic Diseases / Peking University Institute of Hematology
Professor Huang is an Academician of the Chinese Academy of Engineering, Chief Physician, and PhD supervisor. He serves as Director of the National Clinical Research Center for Hematologic Diseases, Director of the Peking University Institute of Hematology, and Head of the Department of Hematology at Peking University People’s Hospital. He is also President of the Institute of Medical-Engineering Translational Research at the same hospital.
He has received numerous prestigious awards, including the Ho Leung Ho Lee Science and Technology Progress Award, the Guanghua Engineering Science and Technology Award, the Shulan Medicine Award, the Distinguished Service Award jointly conferred by the Center for International Blood and Marrow Transplant Research (CIBMTR) and the American Society for Transplantation and Cellular Therapy (ASTCT), and the International Collaboration Contribution Award from the International Society of Hematology.


