
The 2026 European Association of Urology Annual Congress (EAU26), one of the most prestigious global meetings in urology, brought together leading advances in urologic oncology. Multiple studies on precision diagnosis of prostate cancer from the team led by Prof. Kan Gong and Prof. Yi Liu at Peking University First Hospital were selected for presentation, showcasing contributions from Chinese researchers on the international stage. Oncology Frontier invited Prof. Gong to share detailed insights into these findings. 01
Congratulations on having multiple prostate cancer studies selected for presentation at EAU 2026. Could you walk us through the key findings and major highlights from your team’s work?
Prof. Kan Gong:
At this year’s EAU meeting, several of our studies focusing on precision diagnosis and management of prostate cancer were presented. China is now entering a deeply aging society, with over 350 million people aged 65 and above. As prostate cancer is a typical malignancy in older men, the importance of early detection and standardized management continues to grow.
Currently, the five-year survival rate for prostate cancer in China is approximately 67%, whereas in developed countries it reaches around 97%. This gap highlights substantial room for improvement in early diagnosis and treatment.
In our daily clinical practice, we observe that only a small proportion of newly diagnosed patients are at an early stage suitable for curative treatment, while the majority already present with advanced disease. This underscores the urgent need to improve early detection and precise staging.
Our research is therefore driven by real-world clinical challenges. One major focus has been optimizing prostate biopsy strategies, which remain the cornerstone of diagnosis. Although recent EAU guidelines recommend combining perilesional biopsy with targeted biopsy for MRI-visible lesions, this recommendation is still based on relatively low-level evidence and lacks robust data from Chinese populations.
To address this, we collaborated with Prof. Yi Liu and Dr. Ruiyi Deng to conduct a randomized controlled trial (PERI-PRO RCT), comparing perilesional plus targeted biopsy with the conventional systematic plus targeted biopsy approach. At this meeting, we presented a secondary analysis of this trial.
The results showed that, in patients with a single suspicious lesion on multiparametric MRI (mpMRI), perilesional plus targeted biopsy achieved non-inferior diagnostic performance compared with the conventional approach, while significantly reducing the number of biopsy cores. On average, this strategy reduced six biopsy samples per patient.
Clinically, this is highly meaningful. It maintains diagnostic accuracy while reducing unnecessary tissue sampling, thereby lowering procedure-related trauma and complication risks.
Further spatial analysis demonstrated that, when effective targeted biopsy is performed, the additional diagnostic yield from perilesional sampling and ipsilateral systematic biopsy was modest but relevant, at 4.2% and 4.7%, respectively. In contrast, contralateral systematic biopsy provided no additional diagnostic benefit and increased the detection of clinically insignificant cancers.
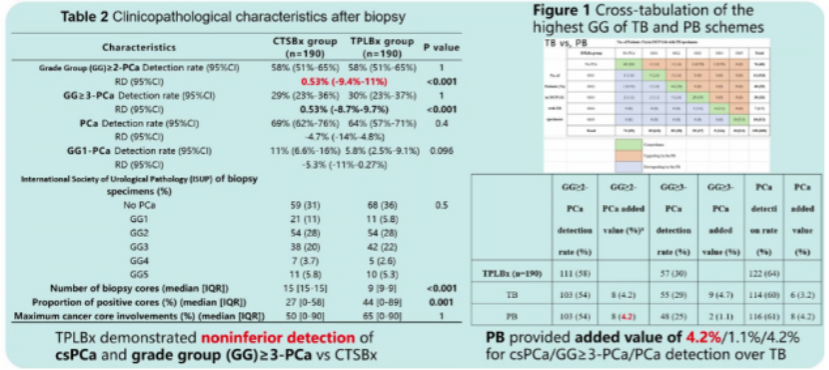
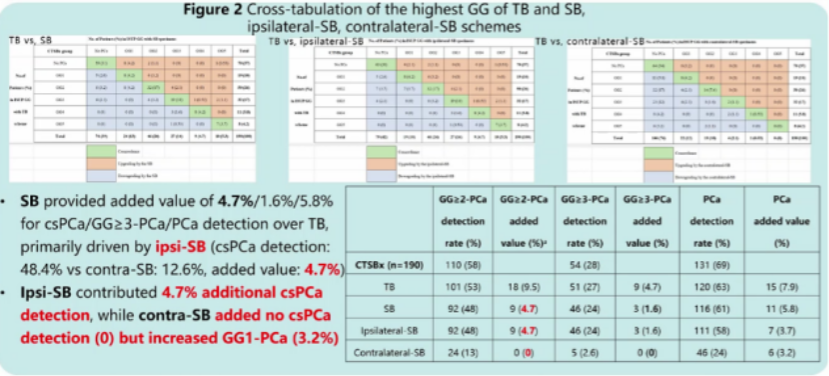
This study provides high-level evidence for optimizing biopsy strategies and advancing individualized precision diagnosis in prostate cancer. We are currently conducting a multicenter randomized trial in China and hope that future results will contribute to updates in international guidelines, as well as inform national clinical practice by offering a China-based solution to improve diagnostic accuracy while minimizing patient burden.
02
Another study from your team, focusing on transition zone PSA density (PSAD) and artificial intelligence, was also presented at this meeting. Could you elaborate on its findings and clinical implications?
Prof. Kan Gong:
At the session on urologic technology, complications, artificial intelligence, and prostate cancer outcomes, we presented our research—led by Dr. Jiaheng Shang in collaboration with Prof. Yi Liu—on the use of transition zone PSAD to assess the risk of clinically significant prostate cancer (csPCa) in patients with negative mpMRI.
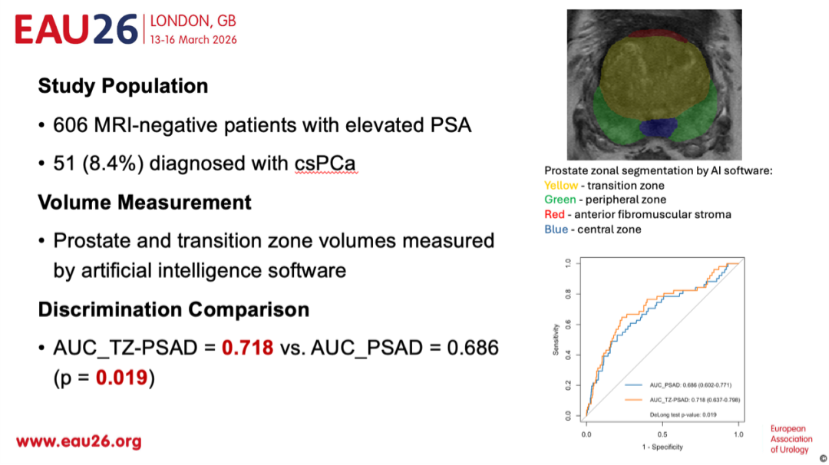
This study addresses a very common and challenging clinical scenario. Many patients present with elevated serum PSA levels but negative mpMRI findings, and the key question becomes whether a biopsy is still necessary. Accurately identifying which patients truly require biopsy remains a major unmet need.
To tackle this issue, we incorporated artificial intelligence–based imaging analysis to precisely identify the prostate transition zone and calculate transition zone PSAD.
Our results demonstrated that AI-derived transition zone PSAD significantly outperformed conventional whole-gland PSAD in predicting clinically significant prostate cancer. Based on this metric, a subset of patients could safely avoid unnecessary systematic biopsy.
This approach has strong clinical value as a triage tool, helping to identify high-risk patients who truly require invasive diagnostic procedures while sparing low-risk individuals from unnecessary interventions.
Importantly, this study validates a more targeted, non-invasive imaging biomarker and highlights the role of artificial intelligence in enabling precise quantitative imaging. By improving the accuracy of non-invasive risk stratification, this strategy has the potential to substantially reduce unnecessary biopsies, optimize clinical workflows, and move prostate cancer diagnosis toward a more precise and individualized paradigm.


Prof. Kan Gong

Prof. Yi Liu


