
Editor’s Note: The 2026 American Society of Clinical Oncology Genitourinary Cancers Symposium (ASCO GU 2026) has successfully concluded, delivering multiple landmark advances that are reshaping clinical practice in urologic oncology. In the field of urothelial carcinoma, Professor Hai-Long Hu’s team from Tianjin Medical University Second Hospital presented six high-quality studies spanning organ-preserving strategies, treatment optimization, and liquid biopsy–guided precision management. These studies collectively contribute important evidence to both Chinese and global clinical practice.
During the meeting, Oncology Frontier – UroStream invited Professor Hai-Long Hu, together with Professor Chong Shen and Professor Yun-Kai Xie, to share insights into the TRUCE research program and its clinical implications.

The TRUCE Program: A Full-Course Precision Strategy for Urothelial Carcinoma
Professor Hai-Long Hu: At this year’s ASCO GU meeting, significant advances were reported in urothelial carcinoma worldwide. Our team has long focused on precision diagnosis and individualized treatment, covering surgical innovation, clinical research, and translational studies. Together with Professor Yun-Kai Xie and Professor Chong Shen, we are pleased to share our latest work.
While many groups have contributed substantially to the diagnosis and treatment of NMIBC and MIBC, our research centers on the TRUCE program. The name “TRUCE” reflects our goal of achieving a balance between tumor control and patient well-being through precise, low-toxicity treatment strategies.
The program began with the TRUCE-01 study, which explored neoadjuvant and bladder-preserving strategies in MIBC using low-dose nab-paclitaxel combined with immunotherapy. This approach demonstrated both strong efficacy and favorable safety. Building on this foundation, the TRUCE-02 study targeted patients with very high-risk NMIBC who are not amenable to TURBT. Preliminary results showed durable tumor control, with a large proportion of patients avoiding cystectomy and maintaining long-term responses.
We subsequently expanded the program to include UTUC, designing TRUCE-UTUC 01, 02, and 03 based on tumor location and clinical characteristics. In parallel, we developed the TRUCE-LB series focusing on liquid biopsy and minimal residual disease. Altogether, these studies form a comprehensive framework covering the entire disease spectrum—from early to advanced stages, and from diagnosis to long-term management.
At ASCO GU 2026, we presented six studies. Three focused on utDNA liquid biopsy, while the remaining studies addressed organ-preserving UTUC strategies, the relationship between renal function and immunotherapy response, and optimization of low-dose chemotherapy combined with immunotherapy.
Clinical Studies: Advancing Precision Treatment Strategies
Professor Chong Shen: Among the studies presented, three clinical investigations focused on optimizing treatment strategies for urothelial carcinoma.
The TRUCE-UTUC 01 study explored a neoadjuvant approach combining a PD-1 inhibitor with an anti-HER2 antibody–drug conjugate in patients with HER2-positive distal ureteral carcinoma. This population is particularly suitable for kidney-sparing surgery. The results were encouraging: nearly half of the patients achieved pathologic complete response, and the majority experienced significant tumor shrinkage. Importantly, no deaths were observed during follow-up, and adverse events were generally mild. This strategy demonstrated that effective tumor control can be achieved while preserving renal function.
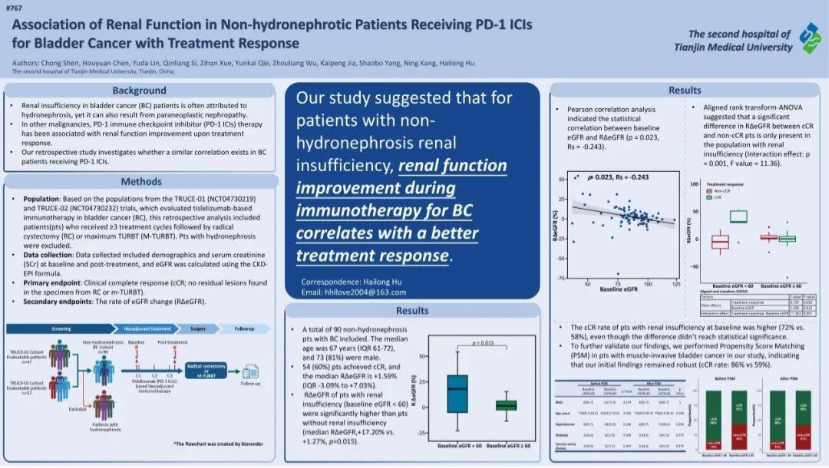
Another study examined the relationship between renal function and response to immunotherapy in bladder cancer patients without hydronephrosis. We observed that patients with baseline renal impairment showed greater improvement in renal function during treatment, and this improvement was closely associated with better therapeutic response. Interestingly, these patients also had higher complete response rates, suggesting that renal function dynamics may serve as a clinically useful biomarker.
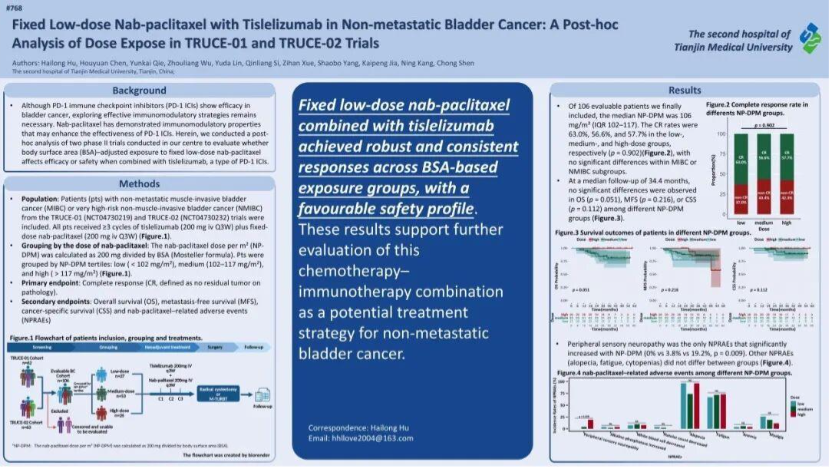
We also evaluated a simplified dosing strategy using fixed low-dose nab-paclitaxel combined with immunotherapy. Unlike conventional dosing based on body surface area, this approach aims to maintain efficacy while reducing toxicity. Our analysis showed consistent treatment outcomes across patients with different body sizes, with no significant differences in survival endpoints. These findings support the feasibility of simplifying treatment regimens without compromising efficacy.
Liquid Biopsy: Enabling Non-Invasive, Full-Course Management
Professor Yun-Kai Xie: We also presented three studies focusing on urinary tumor DNA (utDNA), exploring its role across the entire disease course of bladder cancer.
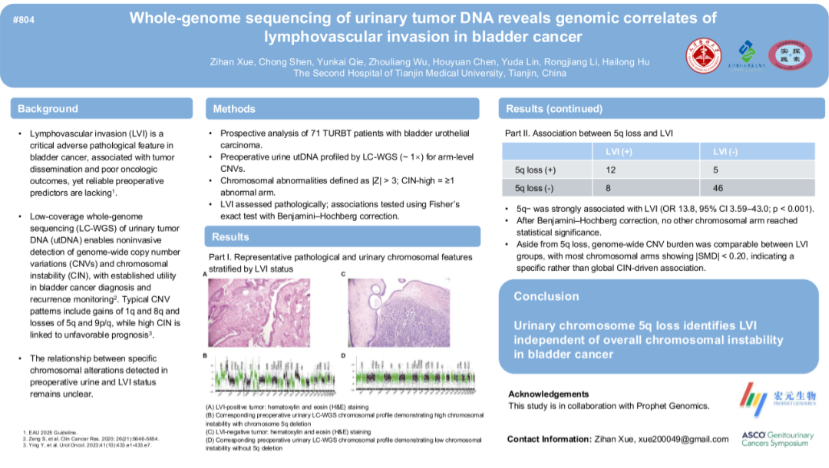
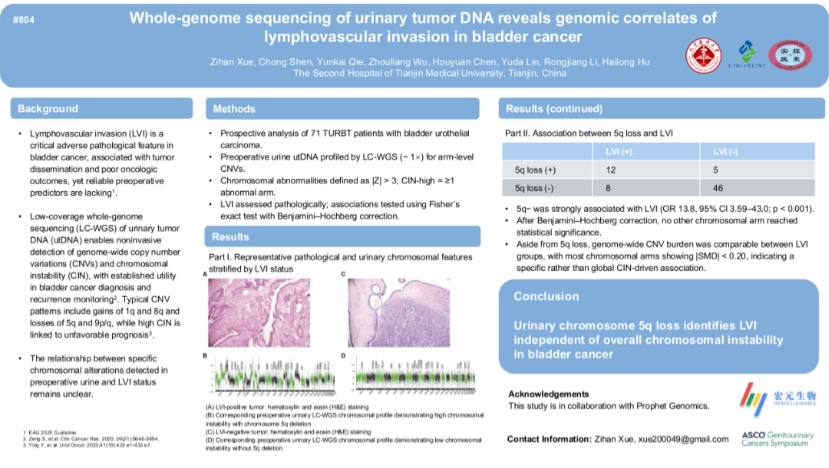
In the preoperative setting, we identified a strong association between chromosome 5q deletion detected in utDNA and lymphovascular invasion. This finding enables non-invasive risk prediction before surgery and may help guide treatment planning.
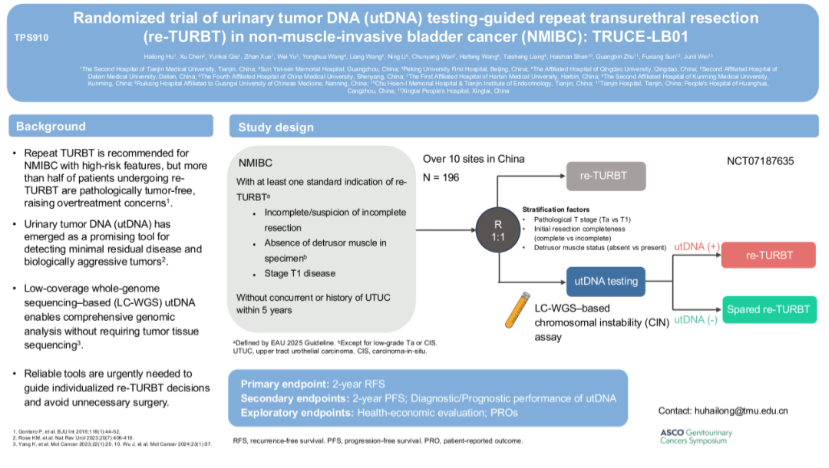
In the perioperative setting, we are investigating whether utDNA can guide the need for repeat TURBT. Current guidelines recommend routine second resection in certain patients, yet many ultimately have no residual tumor. Our data suggest that utDNA can accurately predict residual disease, raising the possibility of avoiding unnecessary procedures in selected patients.
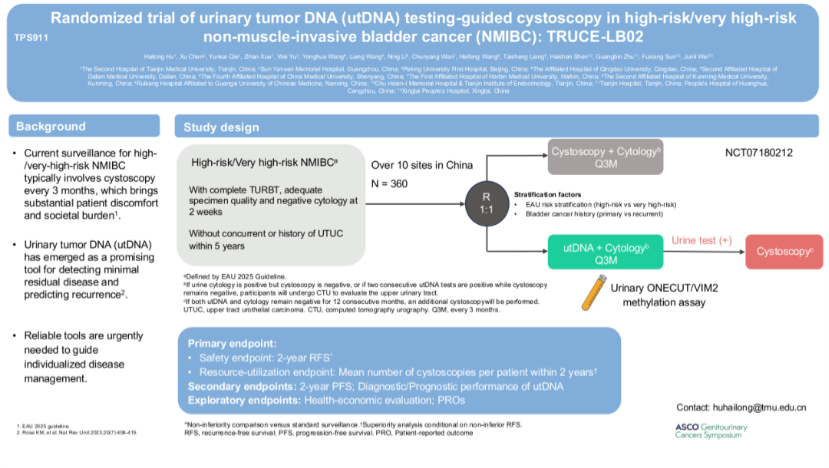
In the postoperative setting, we are evaluating a utDNA-guided surveillance strategy. Instead of performing cystoscopy at fixed intervals for all patients, this approach proposes that only utDNA-positive patients undergo invasive examination, while utDNA-negative patients can safely defer it. This strategy aims to reduce patient burden while maintaining effective monitoring.
Future Perspectives: Toward Truly Personalized Care
Professor Hai-Long Hu: The central theme of our research is patient stratification. Whether through liquid biopsy or treatment response assessment, our goal is to move beyond one-size-fits-all approaches and enable individualized management.
Professor Yun-Kai Xie: utDNA is rapidly evolving from a diagnostic tool to a platform that can guide treatment decisions. It has the potential to transform clinical practice by enabling earlier risk prediction, more precise treatment selection, and dynamic monitoring.
Professor Chong Shen: Ultimately, liquid biopsy technologies will allow real-time molecular tracking, helping clinicians optimize treatment intensity and timing. This represents a shift toward proactive, personalized care.
Conclusion
The TRUCE program demonstrates how integrating precision therapy with liquid biopsy can reshape the management of urothelial carcinoma. By shifting from procedure-centered to patient-centered care, these strategies aim to achieve optimal tumor control while minimizing treatment burden and improving quality of life.

Professor Hai-Long Hu

Professor Chong Shen

Professor Yun-Kai Xie


