
From March 22 to 25, 2026, the 52nd EBMT Annual Meeting was held in Madrid, Spain, bringing together thousands of experts worldwide to discuss the latest advances in transplantation and cellular therapy. During the plenary session, Prof. Huang He from the First Affiliated Hospital of Zhejiang University School of Medicine delivered a keynote presentation entitled “Armored and In Vivo Next-Generation CARs.” His talk provided a comprehensive overview of two major cutting-edge directions in the field—armored CAR-T cells and in vivo–generated CAR-T cells—highlighting their technological breakthroughs and emerging clinical potential.
Background and Scientific Rationale
Over the past decade, cellular immunotherapy—particularly CAR-T therapy—has evolved from a proof-of-concept into a clinically transformative treatment modality. More than ten CAR-T products have now been approved globally, demonstrating remarkable efficacy in diseases such as acute lymphoblastic leukemia, lymphoma, and multiple myeloma.
Despite these successes, several challenges remain, including relapse and suboptimal responses in certain disease subtypes. To address these limitations, next-generation CAR-T strategies are being developed, with particular focus on two key directions: functionally enhanced “armored” CAR-T cells and in vivo CAR-T approaches.
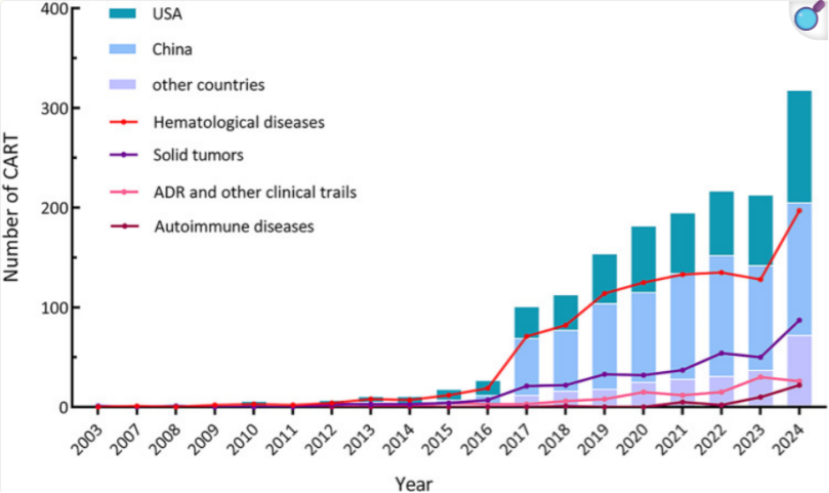
Q1. What clinical needs are driving the development of next-generation CAR-T technologies?
According to Prof. Huang, armored CAR-T cells are designed through genetic engineering to co-express immunomodulatory molecules, thereby enhancing expansion, persistence, and overall antitumor activity. One of the current research hotspots involves integrating metabolically supportive cytokines such as IL-18 or IL-10.
For example, the team led by Carl June reported in The New England Journal of Medicine that IL-18–enhanced CD19 CAR-T (huCART19-IL18) demonstrated promising clinical activity. Similarly, Prof. Huang’s team developed a metabolically enhanced CD19 CAR-T product expressing IL-10 (META10-19), which achieved strong clinical responses using only one-thousandth of the conventional cell dose. This approach not only reduces the required cell quantity but may also eliminate the need for lymphodepleting conditioning in some patients, offering particular advantages in autoimmune diseases.
In parallel, in vivo CAR-T technology represents an even more disruptive innovation. Traditional CAR-T therapy requires a multi-step ex vivo process—cell collection, activation, gene modification, expansion, and reinfusion—which can take several weeks. In contrast, in vivo CAR-T aims to generate CAR-T cells directly within the patient through a single administration, typically using lipid nanoparticles or viral vectors to deliver CAR constructs.
This strategy has the potential to overcome key limitations of conventional CAR-T therapy, including high cost, long manufacturing time, and product variability, moving toward a truly “off-the-shelf” or even “one-shot” treatment paradigm. Early clinical data, such as BCMA-targeted in vivo CAR-T therapy (ESO-BCMA01) reported by Chinese investigators, have already demonstrated feasibility.

Q2. What are the key innovations and clinical implications of these strategies?
Both armored and in vivo CAR-T approaches are built on the same fundamental principle—genetically equipping T cells with chimeric antigen receptors to enable precise tumor targeting. However, they offer significant advantages in manufacturing efficiency, cost reduction, and accessibility.
Armored CAR-T products such as META10-19 exhibit enhanced in vivo expansion and persistence, allowing effective treatment with extremely low cell doses. This simplifies the production process, reduces dependence on large-scale leukapheresis, and broadens patient eligibility.
In vivo CAR-T further streamlines therapy by eliminating ex vivo manufacturing entirely. A single administration can directly generate functional CAR-T cells within the patient, dramatically improving scalability and accessibility.
These approaches have already shown early clinical promise in both hematologic malignancies and autoimmune diseases. Notably, clinical studies led by Chinese research groups have demonstrated strong efficacy and favorable safety profiles, with some results published in high-impact journals such as The Lancet Haematology. In addition, exploratory studies in diseases like systemic lupus erythematosus suggest that effective treatment may be achieved even without intensive conditioning regimens.
Nevertheless, Prof. Huang emphasized that broader clinical adoption will require larger, multicenter studies with long-term follow-up to confirm durability and safety.

Q3. What trends stood out at EBMT 2026 in cellular therapy and transplantation?
Prof. Huang highlighted that hematopoietic stem cell transplantation remains a cornerstone therapy for malignant and refractory hematologic diseases. In the era of precision medicine, the field is increasingly moving toward individualized treatment strategies.
This shift is reflected in several aspects of clinical practice. Patient selection is becoming more refined, incorporating molecular characteristics, prognostic scoring systems, and overall patient condition. Conditioning regimens are evolving from standardized chemotherapy toward combination approaches integrating targeted agents and immunotherapy. Meanwhile, the management of complications—such as graft-versus-host disease, infection, and relapse—is becoming more proactive and biology-driven, supported by molecular monitoring and targeted interventions.
A particularly important emerging theme is the integration of transplantation with CAR-T therapy. How to optimally sequence or combine these two modalities has become a major focus of current research, with multiple studies at EBMT 2026 addressing this question.
Overall, advances in precision transplantation strategies and their integration with cellular therapies are reshaping the field, paving the way for more effective and safer treatment paradigms.


Expert Profile

Prof. Huang He is a Qiushi Distinguished Professor at Zhejiang University and a leading expert in hematology and cellular therapy. He serves as Director of the Bone Marrow Transplantation Center at the First Affiliated Hospital of Zhejiang University and leads multiple national and international research initiatives in stem cell transplantation and immunotherapy.
He has published nearly 200 SCI-indexed papers in top journals including The New England Journal of Medicine, Nature, and The Lancet Haematology, and has received multiple national science and technology awards. His work focuses on translational research in stem cells and next-generation cellular immunotherapies, contributing significantly to the global advancement of the field.

